|
The External Eye Disease clinic is one of the more exciting rotations during our residency in the Department of Ophthalmology in PGH. Our mentor there was a brilliant researcher and teacher who was widely respected for his knowledge and experience. We all looked forward to being mentored by him because we get to see and learn about an enormous number of common and even rare cases just from the sheer number of patients that come to PGH everyday.
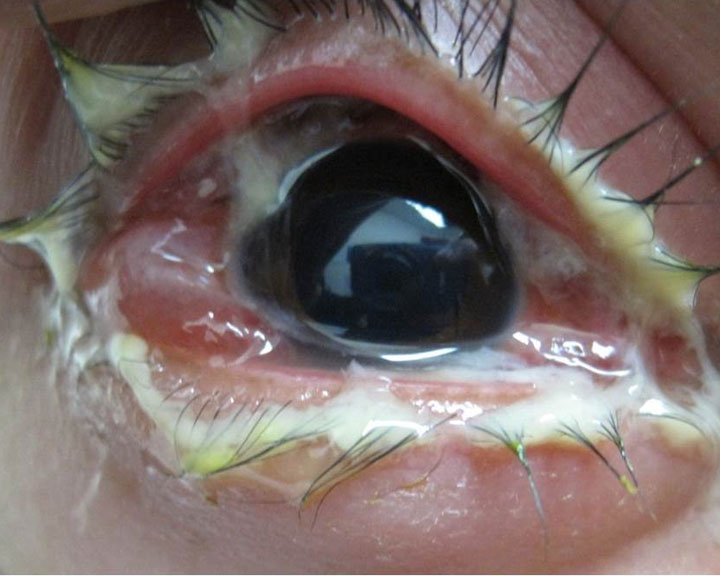
It was here that I saw the case of a girl, barely 2 years old who was brought in by her mother because the child's eyes were covered in pus. The lashes were stuck together and the child was clearly agitated. With one look, Dr. Valenton, our consultant, sadly shook his head, “it’s gonorrhea”. “How is this possible?” I thought. Gonorrhea is a sexually transmitted disease. Was the girl a victim of abuse? No, the mother insisted. Then she claimed that her baby probably just had “sore eyes” or “piskat” because many people in the densely populated urban-poor community where they lived also had “sore eyes”. Piskat is a highly contagious viral infection of the eyes that is transmitted by touching contaminated surfaces or body parts. It is easily passed on among persons who live very close together. And a baby is particularly vulnerable because people love to kiss them. It is not unusual for neighbors and friends to ask to hold the baby or playfully kiss it. Someone with mild sore eyes might have kissed this baby and that's why she also got it. Luckily most cases of “sore eyes” will eventually get better after about a week, even with no treatment. Maybe this child simply had piskat? “Did you drop urine on your baby’s eyes?” Dr. Valenton casually asked the mother. Yes, yes she did, the mother answered. Treating sore eyes with urine is a common practice in many poor communities because it really does seem to be effective. Personal testimonials of people who got well after putting urine were all the proof needed to make the rather gross practice become widely accepted as a cheap form of folk remedy, instead of the expensive eye drops an eye doctor might prescribe. The use of urine and many other folk remedies result from a wrong conclusion about many self- limited viral diseases because they will eventually get "cured" if given enough time. Very often the treatment claimed to be the reason for the “cure” actually had nothing to do with it. It was just the natural course of the condition. Most of the time, these folk remedies are not dangerous. For example people also believe that mother’s breast milk is effective in "sore eyes", but luckily there’s little harm from using that. And for many people, urine is much easier to obtain than mother’s milk, so they use that instead. Again, other than it being rather gross, this is not necessarily wrong - if the urine is “clean”. The danger is if the person who "donated" the the urine happens to have gonorrhea. Then this simple folk remedy becomes dangerous. This is what happened to this child. It was very clear that this baby did not just have “sore eyes”. It looked so much worse. Her lids were swollen, red and fresh pus mixed with the tears coming out of her eyes while she cried. We collected a little bit of her tears and stained it on a glass slide. A quick look under the microscope confirmed Dr. Valenton’s suspicion. The baby had gonorrheal conjunctivitis. Gonorrheal conjunctivitis or GC is a severe bacterial eye infection which, unlike a viral infection, is usually very treatable with antibiotics, although a few strains have developed resistance to the more common ones. This baby was lucky. Her infection responded to the antibiotics and she quickly got well soon after. Like “sore eyes” COVID-19 is a viral infection that easily spreads in densely populated communities; and just like most viral infections, almost everyone who gets it will eventually get well, often with mild or no symptoms. But the very fact that most patients get well even without treatment is also why it is so easy for some people to jump to the wrong conclusion and easily believe that the folk remedy they tried is very effective. More and more people try it and those who get well then become the strongest evangelists and proponents of the remedy. This is why many well-meaning and educated people will swear that “tuob cured them.” They are certain that after doing "tuob", their symptoms disappeared and they got well not realizing that they would have gotten well even if they just rested in bed, stayed hydrated and took some pills for the fever. "Tuob" or the practice of inhaling steam unfortunately may actually make matters worse for the few who will eventually get severely ill; and because they waited too long before getting serious help, they could die. Also, by sharing the communal "tuob", the chances of spreading the infection becomes more likely among the vulnerable members of the family. And even if they don’t actually have the infection, the danger of burns and accidents from using boiling water just can not be ignored. Testimonials and stories are what doctors call “anecdotal evidence”. Time and again this has been shown to be the weakest form of evidence in proving the efficacy of any remedy. It often unknowingly causes more harm than good. The very dangerous pronouncements made by people in government who do not seem to accept that they may be very very wrong about something they are encouraging their constituents to do is the reason why doctors are now raising the alarm about such popular practices. We can not just sit back and let this kind of thinking go unchallenged. I’ve been in practice for 30 years and until now I still don’t understand why people would choose to believe a neighbor, friend, relative or worse, a politician, instead of practically the whole community of doctors. It’s uncanny how a baseless superstition can spread as quickly as a viral infection. It makes many doctors want to give up, or for some to lose control and say things they maybe should not have said out of sheer frustration at the seeming futility of it all. But this does not mean that what they’re saying is wrong. Dr. TK Gonzales Glaucoma Specialist by: Ronald Steven Medalle II An interesting and rare case that I reported during my residency in the DOH-Eye Center of East Avenue Medical Center was published recently in the first quarter 2020 issue of The Asian Journal of Ophthalmology. This case had already been presented at multiple conferences of various Ophthalmologic societies in Manila in the past 2 years. The patient had a history of blunt trauma to the eye that initially presented with bleeding but which had been treated successfully. Later, it was observed that her eye pressures were persistently lower than normal and yet, uncommonly, she had no symptoms. We decided to observe her closely for possible complications. Eventually, she developed a cataract which needed surgery. It was only during the procedure that an abnormal cyclodialysis cleft or an abnormal path for eye fluid to flow was noted. This explained why her eye pressure was persistently lower than normal. By performing an uncommon repair procedure along with cataract surgery the cleft was closed off and her condition resolved. Currently, the patient is doing well with very good vision. Simple blunt trauma to the eye can lead to many complications, some relatively benign as in this case, but not always. Persons who work in hazardous conditions must use protection at all times. I was fortunate to learn about this rare and successfully managed condition during my residency. I'm especially glad the paper was fit for publication in a prestigious international journal.
When we cautiously reopened our clinics 2 weeks ago, we were hopeful that the worst was over and that we could finally get back to serving you for all your eye care needs.
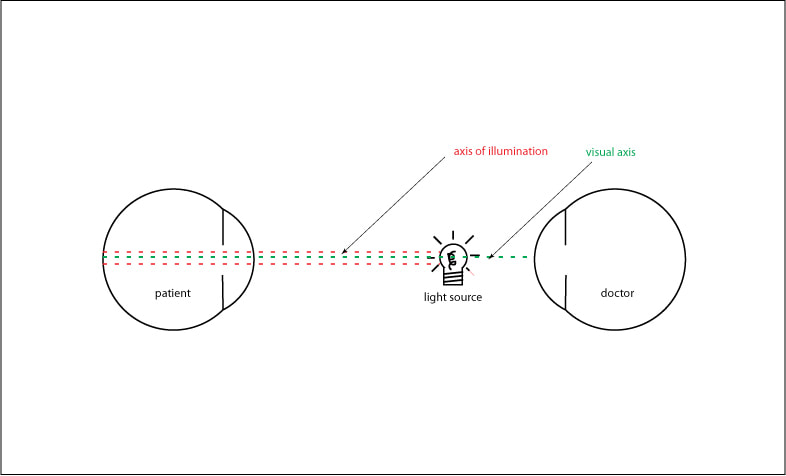
But it quickly became clear that our optimism was unjustified as the number of new cases of COVID-19 in our community surged faster than expected. Just when we thought the worst was over, Cebu finds itself once again facing the threat of an upsurge of COVID-19. We fully understand the decision of the government to return to ECQ as a necessary sacrifice to prevent what could be even more suffering in the days to come. Nevertheless, the members of the ACES Eye Team have all agreed that WE WILL KEEP OUR CLINICS OPEN because many of our patients can no longer delay the treatment they need to prevent losing their sight. We will remain steadfast in our efforts at minimizing the risk of infection for everyone under our care. ACES Eye Clinic will continue to serve you in Perpetual Succor every morning from Monday to Friday and ACES in MAAYO and Dumaguete will continue to be open during regular hours. To check on your doctors schedule, please go to https://www.aceseye.com/clinic-scheduler.html If you are unable to come to the clinic, we are also offering ONLINE CONSULTATION at https://www.aceseye.com/telemedicine.html As a necessary precaution we are asking everyone to please set an appointment before your visit. Yes, we’re scared too but we won’t turn our backs on you. We’re here for good. Today, June 19 is the 159th birthday of our National Hero Jose Rizal. This famous painting above shows Jose Rizal, who trained as an ophthalmologist in Europe in the 1880’s, examining his mother. He is doing a procedure that is still commonly done by all ophthalmologists to this day, albeit with more sophisticated instruments. He is looking at her retina and optic nerve, The retina is an important part of at the eye. It is the innermost layer and it contains the cells that are able to detect light and transform it into nerve impulses which in turn is sent to the brain, allowing us to see. Being such an essential part of the eye, it is very important that the retina be examined closely. But, it’s not that easy. Since the retina is located inside the eye and the only opening, the pupil, is less than half a centimeter, the inside of the eye is normally in near or total darkness. To see the retina, the examiner must provide a source light as illumination otherwise it will be too dark to see anything inside. The tiny pupil limits how much light can enter the eye at any given time to protect the light-sensitive retina from being overwhelmed. This is why you instinctively blink or even turn away to avoid the glare when someone flashes a very bight light in front of you and why it is dangerous to look at the sun directly. To make things even harder, the examiner has to peer through the same pupil as that of the source of light, so his line of sight will necessarily have to be in the same path. In other words his line of sight as well as the light source have to be on the same axis, or are coaxial. (see fig.1) In the painting, the source of light is behind his mothers head. Rizal is holding with his right hand a small concave mirror with an opening in the center. This reflects and focuses the light into a narrow beam that is then directed to the inside of the eye through the pupil. The image of the retina is visible on the condensing lens that he holds in his left hand. Since he is looking through the opening in the center of the concave mirror, his line of sight is now co-axial with his examining light. Nowadays ophthalmologists, and especially retina specialists still use similar instruments that rely on the same principle albeit more sophisticated thus making the procedure much easier to perform and with less discomfort for the patient and the examiner.
Examining the retina is a very important in a lot of diseases because it allows the eye specialist to see in real life the actual condition of the blood vessels and nerves inside our bodies which otherwise would not be visible. Retina specialists are highly skilled in peering deep inside the eye and enables them to see such conditions as retinopathy of prematurity, ARMD, diabetic retinopathy, retinal detachment, vitreous hemorrhage and many more. Glaucoma specialists and neuro-ophthalmologists also rely on this to see status of the optic nerve. In a way, it allows us a peek into the human brain.  The Trail We Blaze by Dr. Stacey Aquino-Cohitmingao One of my earliest memories was of mini scrub suits. In the late 80’s, little scrubs were not common. My brother and I would wear them and our parents would bring us around to the hospital. Sometimes we would wait in the lounge, while our dad did his surgeries. My child-like brain knew two things: he was good at what he did, and that he was respected among his peers. We fast forward to the time when I was I had just passed the Philippine Physician’s Licensure Examination. The question was never “what specialty shall we choose for training?” but “which residency training in Ophthalmology are we going into?” There was no other option. It came down to a choice between my father’s alma mater, the Philippine General Hospital, and the Cebu Velez General Hospital, where he was the immediate past Chairman of the Department. In the end, the decision was made to have my education in close proximity to him, so that he may have a hand in teaching me the skills needed for microsurgery. Residency was a confusing time. Everyone around me thought that I would get special treatment, being the daughter of the Chairman of the Department. The truth, like most children of doctors will tell you, is that I had a worse time than most. Everyone expected a certain level of performance from you. They expected you to be exactly like your father. On more than one occasion, I was treated rather unfairly; because everyone expected me to get special treatment, they would go out of their way to make things difficult for me, so I “wouldn’t get spoiled”. It didn’t matter that none of these people knew who I was, it was easier to make the assumption. This mind space, combined with my initial lack of interest in the specialty, made me resent Ophthalmology as a whole. But here I was, a first year resident in Ophthalmology. It seemed to me that I had 2 choices: spare myself the grief, and transfer to another specialty; or be master of this one so that all prior accusations would sound ridiculous. Everyone had a different goal in training. Mine was competence and meticulosity. I knew I wasn’t the most brilliant of students, but I was a dry sponge, and I was ready to absorb everything they were willing to teach me. I would make extra efforts in the subjects that were either uninteresting or complicated. The way I saw it, a lazy genius is worth nothing. The phrase is “Stand on the shoulders of giants”- most people think it’s to give you leverage, so you can see higher than what you’re currently able to. When I think about it, some people are able to stand on the shoulders of giants. Their responsibility is to make sure that they use their time there wisely, to further learning and achievement; but also, to make sure they know how to balance, so they don’t make the giant fall. My father blazed an amazing trail, it is my responsibility to keep it going. It started as a blurred area just a little off the center of my vision, enough to be noticed but not that alarming, I thought. I had similar symptoms before and they disappeared on their own after a while. But this time, it did not. Instead it became steadily worse that by the time I was seen by the retina specialist, it was too late. Age-related macular degeneration or ARMD was the diagnosis, the same condition my father had though his came at a much later point in his life. If I had taken my symptoms more seriously and asked for help sooner, it is possible I could have have ended up with less visual loss.
Macular degeneration treatment breakthroughs inspire hope that someday we may see a cure to this disease. Promising treatments depend upon the stage of disease progression. Learn more about ARMD here |
Aces CaresOur Stories Archives
February 2021
Categories |
||||||
WORLD-CLASS EYE CARE IN THE HEART OF THE PHILIPPINES
|
What Our Clients Are Saying"experience ko very affordable! you are not checked by one doctor only, but by every specialist they have!!, i had cataract at age 52, the examining doctor suspects i may develop glaucoma so he had me checked by their glaucoma specialist. when i complained of dryness in the eyes, another specialist examined me. btw, i was initially examined and operated on by a retina specialist of theirs all went well!!"
Brought my mom there for removal of cataract... Our experience with this clinic and with Dr Aquino who was mom's surgeon was nevertheless outstanding..." "I was here years back...The doctors who attended to me were very accomodating and were even able to build well a doctor-patient relationship..."
photo: Arambulo
|






 RSS Feed
RSS Feed


